The Lethal Information Gap
The appalling neglect of human life continues unabated, as physicians fail to prescribe drugs that could alleviate or cure disease.
One example of an overlooked drug is cimetidine (Tagamet®). In 1985, The Life Extension Foundation recommended cimetidine as an adjuvant cancer therapy. Back then, cimetidine was a prescription drug. Regrettably, most oncologists refused to prescribe it, even though we provided scientific abstracts substantiating its efficacy.
In a landmark study just released by the British Journal of Cancer, patients with an aggressive form of colon cancer showed a remarkable 84.6% survival rate when treated with cimetidine compared to only a 23.1% survival rate for those not treated with cimetidine.[1] This new study shows that cimetidine improved 10-year survival by almost four-fold!
This is not an isolated report. Since the late 1970s, numerous studies have demonstrated the anti-cancer effects of cimetidine, but because the drug was not “approved” as a cancer therapy, most oncologists did not use it.
Colon cancer will kill 56,000 people in the United States this year. The failure to prescribe this one drug (cimetidine) has resulted in the needless death of thousands of Americans annually.
Now, anyone can obtain cimetidine
Cimetidine is no longer a prescription drug. You can buy it right off the pharmacy shelf under the Tagamet® label or less expensive generics (that say “Cimetidine” on the box).
Cimetidine has shown efficacy against many types of cancer. In the most recent study, however, it was only effective against certain forms of colon cancer. A full report about the use of cimetidine by colon cancer patients can be found in the “Cimetidine and Cancer” article that appears in this month’s issue.
While anyone can now obtain low-cost cimetidine, there are additional anti-cancer drugs that require a prescription, and some are outrageously expensive.
The cancer cost crisis
Optimal cancer treatment can require many expensive drugs. For instance, cancer cells thrive in a low oxygen environment, and many cancer patients are anemic.[2-4] According to a recent study published by the American Cancer Society, anemia increases the overall risk of dying from cancer by an astounding 65%![4]
Life Extension long ago recommended that cancer patients increase their red blood cell count, hemoglobin and hematocrit to the upper range of normal in order to boost the oxygen carrying capacity of their blood. Procrit is a prescription drug that increases blood oxygen-carrying capacity.
One study evaluated advanced head-neck cancer patients. Those with hemoglobin below 14.5 had only a 17% complete response and a 62% two-year survival rate. When Procrit was administered to a similar group, there was a remarkable 61% complete response and a 93% two-year survival rate. Procrit thus enhanced the complete response by 3.5-fold and two-year survival by 33%.[5]
Procrit often costs $1500 to $2000 a month and many cancer patients need to take it for many months. Even though Procrit is approved to treat cancer-associated anemia, insurance companies are demanding that cancer patients must first demonstrate severe anemia (20% to 25% below the bottom normal range) before paying for the drug. This means that most cancer patients do not receive Procrit until they are seriously impaired by their disease. In many cases, Procrit should be initiated upon the diagnosis of cancer and not wait for advanced stage disease to develop.*
In case you think that a blood transfusion (to increase red blood cell count) would be a low cost alternative to Procrit, please know that blood transfusions can suppress the immune system. Weakened immune function enables cancer to rapidly proliferate in the body, so blood transfusions are not a solution for cancer patients. Using Procrit improves the quality of life, increases hemoglobin levels and reduces transfusion requirements even when chemotherapy is being used.[6-9]
Speaking of the immune system, the FDA long ago approved a drug called Leukine. This drug partially restores immune cell production lost to the toxic effects of chemotherapy. What few oncologists understand is that Leukine works better when administered concurrently with chemotherapy, rather than waiting to see how much immune damage is inflicted after multiple chemotherapy sessions.[10-12] The primary benefit of Leukine is to stimulate macrophage production to prevent bacterial infection in the chemotherapy patient. Macrophages also engulf cancer cells and assist in their destruction by the immune system.[13]
Since the FDA has only approved Leukine for use after chemotherapy has damaged the immune system, insurance companies aren’t paying for this drug to be administered during chemotherapy. Depending on the dose, it can cost over $1500 a month for Leukine. (Note: Leukine should not be used during radiation.)
Bone loss fuels cancer cell growth
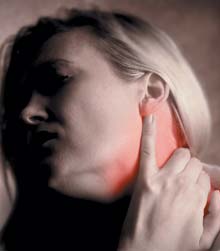
Some types of cancer (breast and prostate) have a proclivity to metastasize to the bone.[14-15] The result may be bone pain which also may be associated with weakening of the bone and an increased risk of fractures.[16-17]
 |
|
PROCRIT versus NO PROCRIT
in Head-Neck Cancer Patients With Hemoglobin in the Lower Range of Normal
|
Complete Response to Chemo-Radiation Therapy |
Two-Year Survival |
| Procrit (Hemoglobin initially below 14.5) |
61% |
93% |
| No Procrit (Hemoglobin below 14.5) |
17% |
61% |
What made this study interesting was that it showed that boosting blood oxygen-carrying capacity to the high normal range was enormously beneficial. Since most of these cancer patients were not anemic, they would not typically have been eligible to receive Procrit. | |
Patients with prostate cancer, for example, are found to have a very high incidence of osteoporosis even before the use of therapies that lower the male hormone testosterone.[18] In settings such as prostate cancer, when excessive bone loss is occurring, there is a release of bone-derived growth factors, such as TGFb-1**, which stimulate the prostate cancer cells to grow further.[19-20] In turn, prostate cancer cells elaborate substances like Interleukin 6 (IL-6), which has as one of its main effects the further breakdown of bone.[21-22] Thus, a vicious cycle results: bone breakdown, stimulation of prostate cancer cell growth and production of IL-6 and other cell products, which leads to further bone breakdown.
The intravenous or oral administration of any of the drugs that are called bisphosphonates, such as Aredia®, Zometa® (intravenous), Fosamax® or Actonel® (oral) can be used to stop this vicious cycle. Such agents stop excessive bone breakdown or resorption and favor bone formation.[23-26] Administration of bisphosphonates should be accompanied by an adequate intake of a bone supplement that supplies all the raw materials to make healthy bone. These include calcium, magnesium, boron, silica, vitamin D and K.
The problem that prostate and breast cancer patients face is that bisphosphonate therapy is approved for treatment only after cancer cells have metastasized to the bone and become clinically apparent by a nuclear medicine bone scan.***
If Aredia were administered monthly to those with certain types of cancers, the risk of bone metastasis could be significantly reduced.[27-28] Life Extension recommended bisphosphonate drugs (like those mentioned above) for certain types of cancer patients more than a decade ago. For many cancer patients, it would be ideal to continue bisphosphonate drug therapy a year or longer. Insurance companies, however, do not pay for bisphosphonates until after the cancer has metastasized to the bone.
Procrit, Leukine and bisphosphonate-class drugs can save the lives of many cancer patients. The high cost of these drugs, however, often precludes their use. We have previously reported that FDA over-regulation is the culprit behind outlandish drug pricing.[29-30]
Less expensive cancer drugs
|
FDA Too Slow
To Approve New Drugs
A new nationwide poll of cancer specialists sponsored by the Competitive Enterprise Institute (CEI) finds many of them believe the FDA is too slow in approving new medical drugs and devices.
CEI’s poll is being released as the agency’s drug approval process once again becomes the subject of much debate, with some arguing that drugs are being approved too quickly, while others believe skyrocketing costs and regulatory barriers are affecting drug
development. The recent controversy over the FDA’s rule for testing pediatric drugs may add another regulatory hurdle to the process. Highlights of the poll include:
 |
Almost two-thirds (61%) of the cancer specialists polled believe the FDA is too slow in approving new medical drugs and devices. |
 |
When doctors were asked if FDA regulations helped or prevented them from using promising new drugs or medical devices in the treatment of their patients, there was an almost even split. (43% Help, 44% Prevent) |
 |
Almost eight out of 10 (77%) responded that the FDA’s approval process has hurt their ability to treat their patients with the best possible care at least once in their medical careers. |
 |
Almost two-thirds (70%) believe the general public doesn’t understand the “human cost” of the FDA approval process—that some people may suffer or die waiting for the agency to act. |
 |
More than half (58%) say the FDA should not restrict information on the use of approved drugs or devices for other unapproved uses, also known as “off-label” uses. |
U.S. Senator Bill Frist (R-TN), co-sponsor of legislation in 1997 to reform the FDA, made this statement regarding CEI’s poll: “What used to take several years has now been reduced to an average review time of six to 10 months for new drugs. Yet, as many respondents indicated, more needs to be done to further improve the drug review process.”
The entire poll can be read online at www.cei.org. The survey—the fifth on this topic sponsored by CEI since 1995—was conducted by the polling company. It included 160 cancer specialists, with a margin of error of +5.1% at the 95% confidence level.
CEI is a non-profit, non-partisan public policy group dedicated to the principles of free enterprise and limited government. For more information about CEI, please visit their website at www.cei.org.
Reprinted courtesy of the Competitive Enterprise Institute, www.cei.org. | |
Not all cancer drugs are cost prohibitive, but oncologists are ignoring their potential value anyway. In 1996, Life Extension recommended that most cancer patients take a COX-2 inhibiting drug because of solid evidence that cancer cells use the COX-2 enzyme as a biological fuel to sustain their rapid division. Back in 1996, Americans had to import a COX-2 inhibitor named nimesulid from other countries, because this class of drug was not widely available in the U.S.
Now that COX-2 inhibiting drugs like Celebrex® or Vioxx® have been approved, scientists in the United States are hard at work to prove that this class of medication prevents cancer and perhaps even cures it.[31-44]
What has scientists so excited is that experiments in lab animals strongly suggest that drugs like Celebrex could help cure cancer, especially if combined with chemotherapy or radiation.[45-47] One scientist estimates there are 100 separate cancer studies involving COX-2 inhibitors at this time going on worldwide.
According to an Associated Press news release on March 30, 2002, doctors are predicting that COX-2 inhibiting drugs may become standard therapy in five to 10 years. There was adequate evidence in 1996, however, to recommend COX-2 inhibiting drugs to cancer patients.
Certain types of cancer cells respond well to statin drug therapy. In advanced primary liver cancer patients, those who received 40 mg of pravastatin survived twice as long compared to those who did not receive this “statin” drug.[48] Statins interestingly are also associated with preservation of bone structure and improvement in bone density.[49-51]
The problem remains that mainstream oncologists are ignoring published findings and are still not prescribing statins, COX-2 inhibitors and other drugs to cancer patients who could benefit. Life Extension members learned about the anti-cancer effects of these drugs many years ago.
Why these lifesaving therapies are ignored?
There are many reasons why the best drugs don’t make it into the bodies of those in need. Sometimes the drugs are too expensive and insurance companies won’t pay for them.
In other cases, doctors are too busy practicing “assembly line” medicine and are not keeping up with the latest research findings. Many doctors don’t want to risk the potential liability involved in prescribing a drug that is not recognized by their peers. These cowardly physicians would rather see their patients suffer agonizing deaths instead of prescribing drugs that are documented in published studies to have potential life-saving effects.
The FDA restricts drug companies from advertising “off-label” benefits of existing drugs. It is cost-prohibitive to obtain FDA approval to make a new disease claim for an existing drug, especially for drugs that do not have long-term patent protection.
The sheer volume of new medical findings is also a problem. It is becoming increasingly difficult for any one doctor to keep up with all the new advances that are announced daily.
 |
| There are many reasons why the best drugs don't make it into the bodies of those in need. Sometimes the drugs are too expensive and insurance companies won't pay for them. In other cases, doctors are too busy practicing "assembly line" medicine and are not keeping up with the latest research findings. | |
Cancer kills 556,000 American every year, or 5.5 million people per decade. Many of these cancer victims are dying needlessly. The fact that cimetidine can drastically reduce the odds of dying from colon cancer is a stark example of the lethal dangers of not being informed.
The study showing that cimetidine dramatically improved survival in certain types of colon cancer was published in a prestigious cancer journal, but the media has not reported on this breakthrough. There are too many of these kinds of medical discoveries that remain buried in scientific journals. The result is that humans who could benefit from this knowledge also wind up buried instead of cured.
As a member of The Life Extension Foundation, you gain access to information today that is not yet recognized by conventional medicine. Our 22-year track record shows that we have been years (if not decades) ahead of mainstream medicine in recommending life-saving therapies.
For longer life,
William Faloon
* Note: The dose of Procrit depends partly on the cause of the anemia and the responsiveness of the patient to initial doses of Procrit. Not all anemias will show a response to Procrit. In patients that may fail Procrit therapy, deficiencies of iron appear to be the main reason. Oral supplementation does not improve the anemia, but intravenous iron does benefit these patients tremendously, especially those with chronic renal failure (Watson A. 1993). The inclusion of intravenous iron reduces the amount of Procrit needed to normalize hemoglobin and hematocrit levels, thereby reducing costs (Glasby J., et al. 1999).
Glaspy J., Cavill I. Role of iron in optimizing responses of anemic cancer patients to erythropoietin. Oncology (Huntingt) 1999 Apr;13(4):461-73; discussion 477-8, 483-8.
Watson A. Iron management during treatment with recombinant human erythropoietin in chronic renal failure. J Clin Pharmacol 1993 Dec;33(12):1134-8.
** Transforming growth factor beta-1.
*** Such a scan picks up metastatic cancer that has spread to the bone when there is sufficient bulky disease within the bone to cause enough increased blood flow that the bone scan can detect disease. More sensitive detection methods that pick up circulating tumor cells in the blood (e.g. RT-PCR technology) or findings of microscopic cancer in the bone marrow (immunological staining for micro-metastases or the use of RT-PCR of marrow specimens) have been published but are not approved as yet by insurance companies. (Diel IJ., et al 1992, 1996)
Diel IJ, Kaufmann M, Goerner R, et al. Detection of tumor cells in bone marrow of patients with primary breast cancer: a prognostic factor for distant metastasis. J Clin Oncol 1992 Oct;10(10):1534-9.
Diel IJ, Kaufmann M, Costa SD, et al. Micrometastatic breast cancer cells in bone marrow at primary surgery: prognostic value in comparison with nodal status. J Natl Cancer Inst 1996 Nov 20;88(22):1652-8.
References
1. Matsumoto S, Imaeda Y, Umemoto S, et al. Cimetidine increases survival of colorectal
cancer patients with high levels of sialyl Lewis-X and sialyl Lewis-A epitope expression on tumour cells. Brit J Can 2002 (86) 161-167.
2. Moliterno AR, Spivak JL. Anemia of cancer. Hematol Oncol Clin North Am 1996 Apr;10(2):345-63.
3. Ludwig H, Fritz E. Anemia in cancer patients. Semin Oncol 1998 Jun;25(3 Suppl 7):2-6.
4. Caro JJ, Salas M, Ward A, Goss G. Anemia of as an independent prognostic factor in survival of patients with cancer: a systemic, quantitative review. Cancer 2001 Jun 15;91(12):2214-21.
5. Glaser, CM, Millesi W, et al. Impact of hemoglobin level and use of recombinant human erythropoietin on response to neoadjuvant chemoradiation therapy, tumor control, and survival in patients with oral or oropharygeal squamous cell carcinoma, Proceedings of the 41st Annual ASTRO meeting, I.J. Radiation Oncology* Biology*Physics, 1999 Vol 45, Number 3 Supp).
6. Glaspy J, Degos L, Dicato M, et al. Comparable efficacy of epoetin alfa for anemic cancer patients receiving platinum- and nonplatinum-based chemotherapy: a retrospective subanalysis of two large, community-based trials. Oncologist 2002;7(2):126-35.
7. Demetri GD, Kris M, Wade J, et al. Quality-of-life benefit in chemotherapy patients treated with epoetin alfa is independent of disease response or tumor type: results from a prospective community oncology study. Procrit Study Group. J Clin Oncol 1998 Oct;16(10):3412-25.
8. Glaspy J, Bukowski R, Steinberg D, et al. Impact of therapy with epoetin alfa on clinical outcomes in patients with nonmyeloid malignancies during cancer chemotherapy in community oncology practice. Procrit Study Group. J Clin Oncol 1997 Mar;15(3):1218-34.
9. Thews et al; Erythropoietin Restores the Anemia-induced Reduction in Cyclophosphamide Cytotoxity in Rat Tumors, Cancer Research, 1998 February 14.
10. Kobrinsky NL; Sjolander DE; Cheang MS; et al. Granulocyte-macrophage colony-stimulating factor treatment before doxorubicin and cyclophosphamide chemotherapy priming in women with early-stage breast cancer. J Clin Oncol 1999 Nov;17(11):3426-30.
11. Pindedo, H.M.; et al The hidden treasures of the primary tumor: Extending neoadjuvant chemotherapy plus GM-CSF in locally advanced cancer. Clinical Cancer Research Vol 6, Nov 2000 (Supp).
12. Baxevanis,C.N., Tsavaris, et al. Granulocyte-macrophage colony stimulating factor improves immunological parameters in patients with refractory solid tumors receiving second-line chemotherapy: Correlation with clinical responses European Journal of Cancer, 1997 Vol 33, No 8, pp1202-1208.
13. Spitler LE. Adjuvant therapy of melanoma. Oncology (Huntingt) 2002 Jan;16(1 Suppl 1):40-8.
14. Waltregny D; Bellahcene A; de Leval X; et al. Increased expression of bone sialoprotein in bone metastases compared with visceral metastases in human breast and prostate cancers. J Bone Miner Res 2000 May;15(5):834-43.
15. Pavlakis N, Stockler M. Bisphosphonates in breast cancer (Cochrane Review). Cochrane Database Syst Rev 2002;(1):CD003474.
16. Plunkett TA, Smith P, Rubens RD. Risk of complications from bone metastases in breast cancer. implications for management. Eur J Cancer 2000 Mar;36(4):476-82.
17. Papapoulos SE, Hamdy NA, van der Pluijm G. Bisphosphonates in the management of prostate carcinoma metastatic to the skeleton. Cancer 2000 Jun 15;88(12 Suppl):3047-53.
18. Berruti A, Dogliotti L, Tucci M, et al. Metabolic bone disease induced by prostate cancer: rationale for the use of bisphosphonates. J Urol 2001 Dec;166(6):2023-31.
19. Shariat SF, Shalev M, Menesses-Diaz A, et al. Preoperative plasma levels of transforming growth factor beta(1) (TGF-beta(1)) strongly predict progression in patients undergoing radical prostatectomy. J Clin Oncol 2001 Jun 1;19(11):2856-64.
20. Reyes-Moreno C, Sourla A, Choki I, et al. Osteoblast-derived survival factors protect PC-3 human prostate cancer cells from adriamycin apoptosis. Urology 1998 Aug;52(2):341-7.
21. Garcia-Moreno C, Mendez-Davila C, de La Piedra C, et al. Human prostatic carcinoma cells produce an increase in the synthesis of interleukin-6 by human osteoblasts. Prostate 2002 Mar 1;50(4):241-6.
22. Paule B. [Interleukin-6 and bone metastasis of renal cancer: molecular bases and therapeutic implications] Prog Urol 2001 Apr;11(2):368-75.
23. Finley RS. Bisphosphonates in the treatment of bone metastases. Semin Oncol 2002 Feb;29(1 Suppl 4):132-8.
24. Harris ST. Bisphosphonates for the treatment of postmenopausal osteoporosis: clinical studies of etidronate and alendronate. Osteoporos Int 2001 Dec;12 Suppl 3:S11-6.
25. Terpos E, Palermos J, Viniou N, et al. Pamidronate increases markers of bone formation in patients with multiple myeloma in plateau phase under interferon-alpha treatment. Calcif Tissue Int 2001 May;68(5):285-90.
26. Berenson JR. New advances in the biology and treatment of myeloma bone disease. Semin Hematol 2001 Apr;38(2 Suppl 3):15-20.
27. Diel IJ, Solomayer EF, Costa SD, et al. Reduction in new metastases in breast cancer with adjuvant clodronate treatment. N Engl J Med 1998 Aug 6;339(6):357-63.
28. Paterson AH. Adjuvant bisphosphonate therapy: the future. Semin Oncol 2001 Aug;28(4 Suppl 11):81-5.
29. FDA Review.org a project of The Independent Institute Why the FDA Has an Incentive to Delay the Introduction of New Drugs http://www.FDAReview.org/incentives.shtml
30. Consumers Against High Prices CONSUMER RAPE February 2002 http://www.stopfda.com/feb2002_economicrape.html
31. Dannenberg A J, Altorki N K, Boyle J O, et al. Cyclo-oxygenase 2: a pharmacological target for the prevention of cancer. Lancet Oncol 2001 Sep;2(9):544-51.
32. Giercksky KE. COX-2 inhibition and prevention of cancer. Best Pract Res Clin Gastroenterol 2001 Oct;15(5):821-33.
33. Ferrandina G, Ranelletti FO, Lauriola L, et al. Cyclooxygenase-2 (COX-2), Epidermal Growth Factor Receptor (EGFR), and Her-2/neu Expression in Ovarian Cancer. Gynecol Oncol 2002 May;85(2):305-10.
34. Cutsem EV, Verslype C, Demedts I. The treatment of advanced colorectal cancer: where are we now and where do we go? Best Pract Res Clin Gastroenterol 2002 Apr;16(2):319-30.
35. Koki AT, Masferrer JL. Celecoxib: A Specific COX-2 Inhibitor With Anticancer Properties. Cancer Control 2002 Mar-Apr;9(2 Suppl):28-35.
36. Kundu N, Fulton AM. Selective Cyclooxygenase (COX)-1 or COX-2 Inhibitors Control Metastatic Disease in a Murine Model of Breast Cancer. Cancer Res 2002 Apr 15;62(8):2343-6.
37. Waskewich C, Blumenthal RD, Li H, et al. Celecoxib exhibits the greatest potency amongst cyclooxygenase (COX) inhibitors for growth inhibition of COX-2-negative hematopoietic and epithelial cell lines. Cancer Res 2002 Apr 1;62(7):2029-33.
38. Husain SS, Szabo IL, Tamawski AS. NSAID inhibition of GI cancer growth: clinical implications and molecular mechanisms of action. Am J Gastroenterol 2002 Mar;97(3):542-53.
39. Kawamoto T, Shoda J, Asano T, et al. Expression of cyclooxygenase-2 in the subserosal layer correlates with postsurgical prognosis of pathological tumor stage 2 carcinoma of the gallbladder. Int J Cancer 2002 Mar 20;98(3):427-34.
40. Hasturk S, Kemp B, Kalapurakal SK, et al. Expression of cyclooxygenase-1 and cyclooxygenase-2 in bronchial epithelium and nonsmall cell lung carcinoma. Cancer 2002 Feb 15;94(4):1023-31.
41. Shaheen NJ, Straus WL, Sandler RS. Chemoprevention of gastrointestinal malignancies with nonsteroidal antiinflammatory drugs. Cancer 2002 Feb 15;94(4):950-63.
42. Xu XC. COX-2 inhibitors in cancer treatment and prevention, a recent development. Anticancer Drugs 2002 Feb;13(2):127-37.
43. Gupta R A, Dubois R N. Colorectal cancer prevention and treatment by inhibition of cyclooxygenase-2. Nature Rev Cancer 2001 Oct;1(1):11-21.
44. Swamy MV, Cooma I, Reddy BS, et al. Lamin B, caspase-3 activity, and apoptosis induction by a combination of HMG-CoA reductase inhibitor and COX-2 inhibitors: a novel approach in developing effective chemopreventive regimens. Int J Oncol 2002 Apr;20(4):753-9.
45. Pyo H, Choy H, Amorino GP, et al. A selective cyclooxygenase-2 inhibitor, NS-398, enhances the effect of radiation in vitro and in vivo preferentially on the cells that express cyclooxygenase-2. Clin Cancer Res 2001 Oct;7(10):2998-3005.
46. Hsueh C, Kelsen DP, Schwartz GK. Selective Inhibition of Cyclooxygenase-2 (COX-2) Enhances Chemotherapy-Induced Apoptosis (Meeting abstract). Proc Annu Meet Am Soc Clin Oncol 1999;18:A606.
47. “Arthritis pills a cancer cure?”, March 30, 2002, Associated Press report on research using COX-2 inhibitors in animal studies.
48. Kawata S, Yamasaki E, Nagase T, et al. The effects of pravastatin on survival in patients with advanced primary hepatocellular carcinoma. A randomized controlled trial. British Journal of Cancer, 2001 Apr 6;84(7):886-91.
49. Pasco JA, Kotowicz MA, Henry MJ, et al. Statin use, bone mineral density, and fracture risk: Geelong Osteoporosis Study. Arch Intern Med 2002 Mar 11;162(5):537-40.
50. Edwards CJ, Russell RG, Spector TD. Statins and bone: myth or reality? Calcif Tissue Int 2001 Aug;69(2):63-6.
51. Edwards CJ, Hart DJ, Spector TD. Oral statins and increased bone-mineral density in postmenopausal women. Lancet 2000 Jun 24;355(9222):2218-9.
|